A Patient's Guide to Perthes Disease of the Hip
Introduction
Perthes disease is a condition that affects the hip in children between the ages of four and eight. The condition is also referred to as Legg-Calve-Perthes disease in honor of the three physicians who each separately described the disease. In this condition, the blood supply to the growth center of the hip (the capital femoral epiphysis) is disturbed, causing the bone in this area to die. The blood supply eventually returns, and the bone heals. How the bone heals determines what problems the condition will cause in later life. Perthes disease may affect both hips. In fact, 10 to 12 percent of the time the condition is bilateral (meaning that it affects both hips). This condition can lead to serious problems in the hip joint later in life.
This guide will help you understand
- what part of the hip is involved
- what causes the condition
- what treatment options are available
Anatomy
What part of the hip is affected?
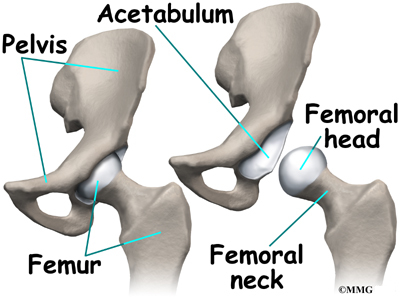
The hip joint is where the thighbone (femur) connects to the pelvis. The joint is made up of two parts. The upper end of the femur is shaped like a ball. It is called the femoral head. The femoral head fits into a socket in the pelvis called the acetabulum. This ball and socket joint is what allows us to move our leg in many directions in relation to our body.
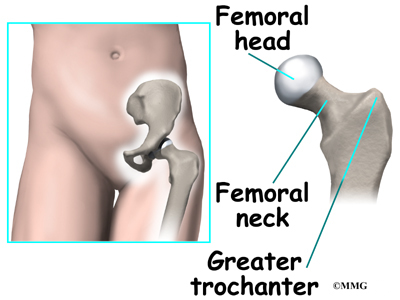
In the growing child, there are special structures at the end of most bones called growth plates. The growth plate is sandwiched between two special areas of the bone called the epiphysis and the metaphysis. The growth plate is made of a special type of cartilage that builds bone on top of the end of the metaphysis and lengthens the bone as we grow. In the hip joint, the femoral head is one of the epiphyses of the femur.
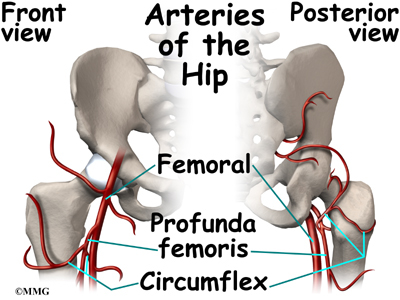
The capital femoral epiphysis is somewhat unique. It is one of the few epiphyses in the body that is inside the joint capsule. (The joint capsule is the tissue that surrounds the joint.) The blood vessels that go to the epiphysis run along the side of the femoral neck and are in danger of being torn or pinched off if something happens to the growth plate. This can result in a loss of the blood supply to the epiphysis. The dead bone cells are eventually replaced by new bone cells but this can take several years. In the meantime, pressure and load from weight on the bone causes the bone to flatten. The smooth, round head of the femur that sets inside the hip socket (acetabulum) becomes oval shaped (ovoid) or misshapen. Instead of fitting tightly inside the acetabulum, bone extrudes or expands outside the confines of the socket.
Causes
How does this problem develop?
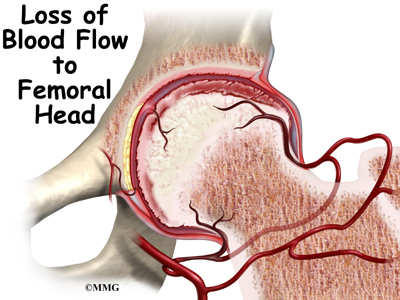
Perthes disease results when the blood supply to the capital femoral epiphysis is blocked. There are many theories about what causes this problem with the blood supply, yet none have been proven. Many experts believe Perthes disease is the result of several or even many factors. Another way to say this is that Perthes is a multifactorial disease with both genetic and mechanical contributing factors.
On the genetic side, it's possible some children are more susceptible (more likely) than others to develop this problem. But it takes one or more "triggers" (environmental or external factors) to start the process. For example, there appears to be some relationship to nutrition. Children who are malnourished are more likely to develop this condition.
Children who have abnormal blood clotting (a condition called thrombophilia) may have a higher risk of developing Perthes disease. These children have blood that clots easier and quicker than normal. This may lead to blood clotting that blocks the small arteries going to the femoral head. As a result of new evidence, the certainty of thrombophilia as a cause of Perthes is now under debate. This will remain an area of study until scientists clear up the significance of thrombophilia as a possible cause of Perthes.
There is some new evidence that Perthes disease is genetic as a result of a mutation (abnormal change) in the type II collagen (fibers that make up soft tissue structures). Previously there was no known increase in risk for children whose parent had Perthes disease as a child. But this belief may no longer be accurate.
Studies among Asian families who have many members with this disease have been found with this mutation in the type II collagen gene. Scientists think that the mutation results in weakening of the hip joint cartilage that also affects the blood vessels within the cartilage.
Other potential biologic factors that may be linked with Perthes disease include low levels of abnormal insulin-like growth factor (IGF-1), low birth weight, and short body length at birth. Exposure to nicotine and other chemicals from tobacco is an important factor recently discovered. Likewise LCP may be triggered by exposure to tobacco if the mother smokes during pregnancy or the child is exposed to second hand smoke during infancy and early childhood.
There is some evidence that Perthes disease can develop after a single episode of ischemia (lack of blood to the area) no matter what the cause. But the risk goes up with repeated (multiple) episodes of blood loss. Whatever the true cause of ischemia (lack of blood to the area), the result is bone death (called necrosis) of the femoral head. Without a normal blood supply, the bone loses its strength and shape. The loss of bone density and softening of the head result in a misshapen head. With the hip supporting the weight of the body, tiny microfractures in the soft, necrotic bone fail to heal. This is another reason why normal wear and tear results in deformity.
The dead bone cells are eventually replaced by new bone cells but this can take several years. In the meantime, pressure and load from weight on the bone causes the bone to flatten. The smooth, round head of the femur that sets inside the hip socket (acetabulum) becomes oval-shaped (ovoid) or misshapen. Instead of fitting tightly inside the acetabulum, bone extrudes or expands outside the confines of the socket. This is another reason why normal wear and tear results in deformity.
Symptoms
What does this problem feel like?
Most children with Perthes disease develop discomfort in the hip and walk with a limp. Children will not usually complain of pain unless specifically asked. The most common way that the disease is discovered is when someone, usually a parent, notices the limp and consults a physician.
When the doctor examines the hip, the motion of the hip is abnormal and restricted. Turning the leg inward produces pain. This usually indicates that the hip is inflamed and may have inflammatory fluid (called an effusion) present in the hip joint.
Interestingly, problems in the hip sometimes do not cause pain in the hip itself. The knee is where the pain is felt. This can be confusing both to patients and physicians. In general, a child with knee pain (who has no clear-cut reason to have knee pain), or an abnormal gait, should be examined for possible Perthes disease. This usually includes X-rays of the hips to make sure that Perthes disease is not missed.
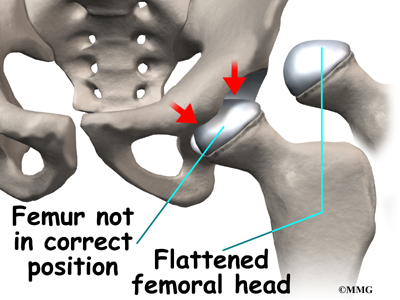
The main problem with Perthes disease is that it changes the structure of the hip joint. How much it affects the way the hip joint works depends on how much the hip joint is deformed. Muscle weakness and atrophy affecting the thigh and calf muscles may develop over time. The affected leg can shorten as a result of the changes in the hip. The result may be a significant leg length difference. Problems later in life are more likely the greater the deformity after the condition has healed.
In general, the most common problem later in life is the development of arthritis in the hip joint. The type of arthritis that develops in the hip is osteoarthritis (also known as wear and tear arthritis). Just like a machine that is out of balance, the hip joint wears out and becomes painful.
Diagnosis
How do doctors identify the problem?
The history and physical examination are usually enough to make the doctor highly suspicious about the diagnosis of Perthes disease. X-rays are usually necessary to make the diagnosis.
It is usually not necessary to get an MRI scan to make the diagnosis. However, this test may be useful to determine whether the other hip is involved in the disease. A special MRI using a dye called gadolinium may help show changes in blood supply before anything shows up on an X-ray.
In planning treatment another test, called an arthrogram, may be required. In this test, dye is injected into the hip joint to outline the cartilage surface of the joint. Much of the child's hip joint is made up of cartilage. Cartilage does not usually show up on X-rays. The dye is necessary to see what the hip will actually look like when the cartilage turns to bone.
Treatment
What treatment options are available?
Age is the determining factor in this condition. Recovery is more likely in children under the age of eight. Development in teens is infrequent but with a poorer prognosis. But the good news is that many children have mild Perthes disease, and they are able to heal and recover fully even without treatment. The hip actually remodels itself and remains smooth moving. Early degenerative hip arthritis does not always occur and these children have no hip problems in adulthood related to their childhood history of Perthes disease.
The primary goal of treatment for Perthes disease is to help the femoral head recover and grow to a normal shape. The closer to normal the femoral head is when growth stops, the better the hip will function in later life. The way that surgeons achieve this goal is using a concept called containment.
Containment is a simple concept. The femoral head can be molded as it heals. This is very similar to molding plastic. Plastic is poured into a molded and held in the mold as it cools. It then holds the shape of the mold. The hip socket, or acetabulum, is not affected when the femoral head loses its blood supply. It can be used as a mold to shape the femoral head as it heals. The trick is that the femoral head must be held in the joint socket (acetabulum) as much as possible. It is better if the hip is allowed to move and is not held completely still in the joint socket. Joint motion is necessary for nutrition of the cartilage and for healthy growth of the joint.
All treatment options for Perthes disease try to position and hold the hip in the acetabulum as much as possible. Giving the hip every opportunity to heal itself by limiting load on the joint may prevent the flattening of the femoral head and deformity that can develop. The only problem is -- it can take two to four years for the necrotic bone to get resorbed and replaced by new bone. And in some cases, new bone never forms. Instead, there is new granulation (healing) tissue, but that area doesn't harden into bone, it just forms cartilage.
Many children who are diagnosed with Perthes disease do not require any treatment except careful watching. When the condition is mild, the results of not doing anything are often as good as aggressive treatment. Active treatment is advised when more than half the epiphysis is affected.
The majority of children who are treated for Perthes disease these days require only a program for maintaining a near-normal range of motion. This may include nighttime splinting, home traction, and physical therapy.Your doctor will determine treatment based on your childs age and a classification of the severity of the disease. The classification is determined by the X-ray findings.
Bracing may be recommended if the child is six years old or younger. Surgery may be a best option for children who are seven or older and who have severe disease. Most of the studies support the idea that treatment of any kind just doesn't seem to make a difference for mild to moderate disease in younger children.
Nonsurgical Treatment
Hip motion, as near to normal as possible, is critical to the successful treatment of Perthes disease. The disease causes inflammation in the joint. This leads to loss of motion and contracture (tightening) of the muscles surrounding the hip joint. Treating these problems to restore normal motion is common.
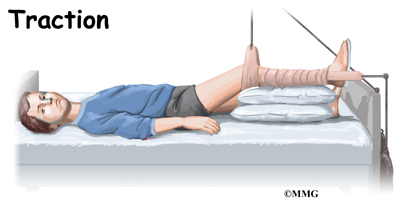
When lack of motion has become a problem, the child may be admitted to the hospital and placed in traction. Traction is used to quiet the inflammation.
Anti-inflammatory medications may be prescribed. Antiresorptive agents may also protect the bone and help decrease deformity. Studies are being done to fully test the effect of these medications in children with Perthes.
Physical therapy is used to restore the hip motion as the inflammation comes under control. This process usually takes about a week. Home traction may also be an option.

In the past, surgeons have tried to hold the hip in the best position where the femoral head was molded by the acetabulum using casts and braces. The most common way of doing this today is the Scottish Rite Orthosis. This brace fits around the waist and thighs and has hinges at the hip joints. The brace allows the child to walk and play while it holds the hip joint in the best position for containment.
Evidence from recent studies have changed our thinking about the usefulness of bracing. Bracing just doesn't seem to change the anatomy or alignment of the hip. There are some children who might benefit but they must be evaluated carefully and selected individually for this type of treatment.
Children who are younger and have significant (more than 50 per cent) of the epiphysis affected may benefit the most from bracing. Children who have chronic synovitis (inflammation of the synovial fluid inside the hip joint) may also benefit from bracing. Holding the hip in place with less load or force helps quiet the inflammatory process.
When X-rays show involvement of the lateral pillar (outside portion of the femoral head), bracing is used to contain the flattened head in the hip socket. The role of bracing is to restore the natural round shape needed for normal hip motion. Results should be followed closely and discontinuation of bracing if no benefit is observed.
Surgery
In some cases, surgery will be required to obtain adequate containment. Sometimes, adequate motion cannot be regained with traction and physical therapy alone. If the condition is longstanding, the muscles may have contracted or shrunk and cannot be stretched back out. To help restore motion, the surgeon may recommend a tenotomy of the contracted muscles. When a tenotomy is performed, the tendon of the muscle that is overly tight is cut and lengthened. This is a simple procedure that requires only a small incision. The tendon eventually scars down in the lengthened position, and no functional loss is noticeable.
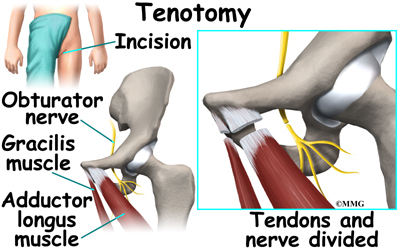
Surgical treatment for containment may be best in older children who are not compliant with brace treatment or where the psychological effects of wearing braces may outweigh the benefits. Surgical containment does not require long-term braces or casts. Once the procedure has been performed and the bones have healed, the child can pursue normal activities as tolerated.
Surgical treatment for containment usually consists of procedures that realign either the femur (thighbone), the acetabulum (hip socket), or both.
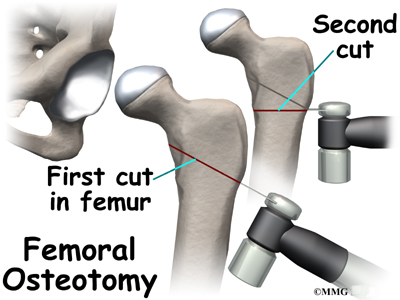
Realignment of the femur is called a femoral osteotomy. This procedure changes the angle of the femoral neck so that the femoral head points more towards the socket. To perform this procedure, an incision is made in the side of the thigh. The bone of the femur is cut and realigned in a new position. A large metal plate and screws are then inserted to hold the bones in the new position until the bone has healed. The plate and screws may need to be removed once the bone has healed.
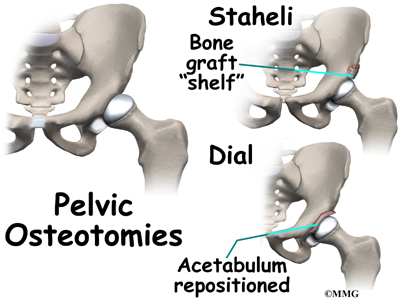
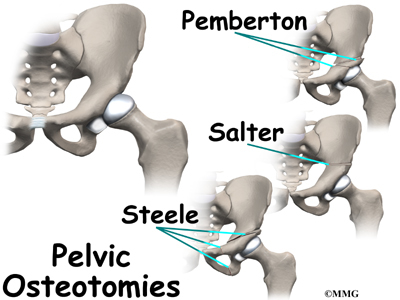
Realignment of the acetabulum is called a pelvic osteotomy. This procedure changes the angle of the acetabulum (socket) so that it better covers, or contains, the femoral head. To perform this procedure, an incision is made in the side of the buttock. The bone of the pelvis is cut and realigned in a new position. Large metal pins or screws are then inserted to hold the bones in the new position until the bone has healed. The pins usually must be removed once the bone has healed.
If there is a serious structural change in the anatomy of the hip, there may need to be further surgery to restore the alignment closer to normal. This is usually not considered until growth stops. As a child grows, there will be some remodeling that occurs in the hip joint. This may improve the situation such that further surgery is unnecessary.
In severe cases, both femoral osteotomy and pelvic osteotomy may be combined to obtain even more containment.
Rehabilitation
What should I expect from treatment?
Follow-up visits are used to monitor the symptoms, hip mobility, and to make sure that the condition is not deteriorating. The surgeon will take X-rays during the recheck visits to follow the healing of the femoral head. Patients with Perthes disease are always at higher risk of developing osteoarthritis of the hip. The more flattened the bone and the more misshapen the round femoral head becomes, the more likely degenerative arthritis will occur at an early age. The reason for this is that joint surfaces need to be evenly matched or congruent. Without this tight fit, the bones rub against each other unevenly. Over time with repeated movements, the joint degenerates where the greatest amount of pressure has been applied.
The end result is that most patients with Perthes disease will require an artificial hip at some point in the future. Most patients do not develop problems for 40 years or more. How soon patients have problems with their hip is directly related to how much deformity is present once the condition heals. In general, the more round the femoral hip is at that time, the longer the hip will stay free of pain.
|




















